Gastroschisis is a rare but significant congenital condition that impacts families worldwide. For expectant parents, hearing a diagnosis of gastroschisis can feel overwhelming, but with advancements in medical care, the condition is now far more manageable than in decades past.
This comprehensive guide will walk you through everything you need to know about gastroshiza, from its causes and treatment options to long-term care and available resources. With greater awareness and understanding, we can create better outcomes for affected children and their families.
What Is Gastroschisis?
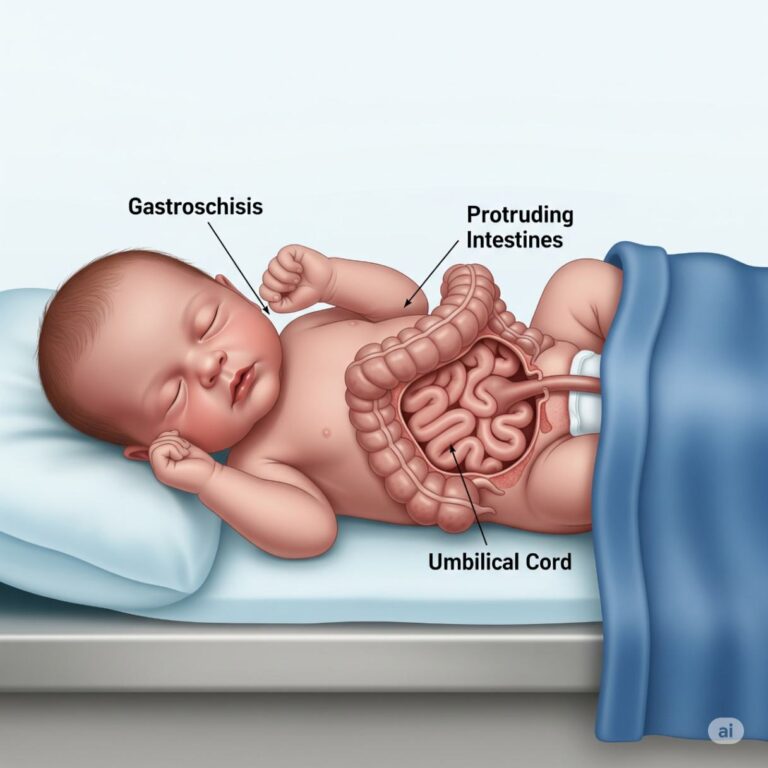
Gastroschisis is a congenital disability in which an infant’s abdominal wall has an opening near the belly button. Through this opening, the intestines (and sometimes other organs) protrude outside the baby’s body without a protective sac. Unlike similar conditions such as omphalocele, the exposed organs in gastroschisis do not have a protective membrane, leaving them vulnerable to irritation and damage.
Types and Severity Levels
While traditional gastroschisis refers to a singular opening in the abdominal wall, there are variations in severity:
- Simple gastroschisis involves only the intestines, with minimal related complications.
- Complex gastroschisis can include additional abnormalities such as narrowing of the intestines, bowel atresia (closed segments of intestines), or severe damage due to inflammation and exposure.
Causes and Risk Factors
The exact cause of gastroschisis remains unknown, but researchers have identified potential risk factors linked to both genetics and environmental influences.
Genetic and Environmental Risk Factors
Gastroschisis seems to occur more frequently in younger mothers under the age of 20, indicating a possible age-related component. Additionally, exposure to certain chemicals, smoking, or substance use during pregnancy may raise the risk.
Maternal Factors
Low maternal body mass index (BMI), first pregnancies, and limited prenatal care often correlate with a higher likelihood of gastroschisis diagnoses. However, most cases happen without any identifiable risk factors, underscoring the need for ongoing research.
Diagnosis and Prenatal Care
Prenatal diagnosis of gastroschisis is typically made through routine ultrasounds, which can show the protruding intestines outside the baby’s body.
Importance of Early Detection
Early detection during pregnancy allows healthcare providers to develop an effective monitoring and care plan. This often includes frequent ultrasounds to assess fetal growth and check for complications such as restricted blood flow to the exposed organs.
Management During Pregnancy
Women carrying a baby with gastroschisis should expect additional prenatal care to ensure both maternal and fetal health. Doctors may recommend maternal-fetal medicine specialists to oversee the pregnancy in collaboration with the primary OB-GYN.
Treatment Options
Gastroschisis requires immediate medical attention after birth, but modern treatment options offer a high survival rate.
Immediate Care After Birth
After delivery, the exposed intestines are covered with a sterile protective material to reduce the risk of infection. The infant is stabilized, and surgeons assess the organs to determine the next steps.
Surgical Procedures
The primary treatment for gastroshiza is surgery to place the intestines and any protruding organs back into the abdominal cavity. This process may occur in stages if the intestines cannot fit into the abdomen immediately. Staged repair involves using a silo (a special protective bag) to reintroduce the organs gradually.
Post-Operative Care
After surgery, babies often require a stay in the neonatal intensive care unit (NICU). They may receive nutrition through intravenous lines while their digestive system heals. Close monitoring helps ensure there are no complications, such as infection or bowel obstruction.
Living with Gastroschisis
While babies born with gastroschisis often require specialized care early in life, most go on to live healthy lives.
Long-Term Health Considerations
Lifelong monitoring may not be necessary for all individuals with gastroschisis, but complications like bowel adhesions or intestinal scarring can occasionally occur. Regular check-ups ensure that any potential issues are addressed promptly.
Nutritional Needs and Feeding Strategies
Infants may initially require tube feeding or specialized formulas until their digestive tract matures. Over time, many transition to regular feeding and achieve normal growth and development milestones.
Physical and Developmental Milestones
Parents should work with pediatricians and physical therapists, if necessary, to monitor development. Most children recover fully and reach milestones like walking, talking, and eating on the same timeline as their peers.
Support and Resources
Families navigating a gastroshiza diagnosis and treatment often benefit from connecting with supportive communities and leveraging available resources.
Organizations and Support Groups
- International Organizations like the March of Dimes provide valuable resources and advocacy for families dealing with congenital disabilities.
- Local support groups (online or in-person) offer a space to share experiences and find encouragement.
Financial Assistance
Coverage for surgeries and long-term care varies by country and healthcare system. Families can explore options like government aid programs, nonprofit resources, or insurance advocacy groups to minimize out-of-pocket expenses.
Awareness Initiatives
Raising awareness about gastroschisis is crucial. Every year, campaigns highlight the challenges of this condition to foster greater understanding and support for affected families.
Research and Future Directions
Ongoing research aims to uncover the underlying causes of gastroschisis as well as improve treatment approaches.
Advancements in Treatment
Innovations like minimally invasive surgical techniques and improved NICU protocols have already enhanced outcomes. Researchers also continue to develop materials and methods to protect exposed organs before surgery.
Future Prospects
By studying the genetic and environmental factors behind gastroshiza, scientists hope to identify prevention strategies. Meanwhile, advances in maternal-fetal medicine may offer improved options for prenatal care and surgical planning.
Personal Stories That Inspire
For families impacted by gastroschisis, hope often lies in the stories of others. Consider the case of baby Alex, who thrived despite a complex gastroshiza diagnosis. His parents credit early diagnosis and a team of skilled doctors for his incredible recovery. Sharing these stories shines a light on resilience and spreads optimism.
The Importance of Awareness and Support
Gastroschisis may be rare, but the courage and resilience of the families navigating it are not. By understanding the condition, supporting research, and fostering community connections, we can improve outcomes for children everywhere.
Raising awareness starts with learning and sharing. If you or someone you know is affected by gastroschisis, connect with trusted organizations today to find guidance and resources.